Malignant transformation of papillary mesothelioma of the tunica vaginalis
SectionUroradiology & genital male imaging
Case TypeClinical Cases
Authors
Natasha Davendralingam1, Asanda Koza1, Rozita Roshani2, Soha El-Sheikh2, Niall Power1, James Bell3
Patient58 years, male
A 58-year-old male non-smoker presented with an irregular painless right testicular lump which gradually increased in size over 10 years. No previous asbestos exposure noted. His GP referred him for ultrasound assessment. On the basis of the ultrasound findings, he was referred to Urology and underwent a surgical excision.
A testicular ultrasound was performed with colour Doppler function. A heterogeneous lesion was identified extending from the right epididymal head into the adjacent tunica vaginalis and testicular parenchyma (4.1cm x 2.7cm x 2.2.cm) [Fig 1]. The lesion demonstrates internal vascularity on colour Doppler. In addition, a cystic area was seen involving the epididymal tail [Fig 2] within which several papillary projections were identified measuring up to 7mm maximally, which also demonstrate internal flow [Fig 3]. The left testicle and epididymis were normal.
Background:
There are only 17 cases of well-differentiated papillary mesothelioma (WDPM) of the tunica vaginalis to date with no documented case of malignant transformation. [1] Only a handful of malignant transformation of WDPM cases have been observed involving the omentum [2, 3], mesentery [4], peritoneum [4] and pleura [5,6]. WDPM originates from mesothelial cells found in the pleura, peritoneum, pericardium or in this case report, from the tunica vaginalis due to its embryologic origin from the peritoneum during testicular descent from the abdomen. [7] Some risk factors for development of this disease include asbestos exposure, chronic hydrocoeles, trauma, radiation and recurrent epididymitis. [8]
Clinical Perspective:
WDPM of the tunica vaginalis typically presents initially with painless scrotal enlargement over a long duration. [1] In the rare case of malignant transformation, radical orchidectomy is the mainstay treatment option. [7] Chemotherapy and radiotherapy have been found to demonstrate little benefit. Ultrasound is the imaging modality of choice as there is no associated radiation risk and the typical characteristics of these tumours (e.g. heterogeneous mass, presence of hydrocele) can be well-delineated on ultrasound. The additional benefit of pulsed colour Doppler enables assessment of internal vascularity.
Imaging Perspective:
The features of malignant mesothelioma or WDPM of the tunica vaginalis are not pathognomonic on imaging. However, key findings on ultrasound that would raise suspicion for this diagnosis are the presence of a hydrocele in association with papillary projections, nodular or irregular masses attached to the tunica vaginalis, a heterogenous mass arising from the scrotal wall and internal vascularity of the mass identified. [9] In most cases, the actual definitive diagnosis is only made post-operatively after excision of the testicular tumour and subsequent histological confirmation. [9]
Outcome:
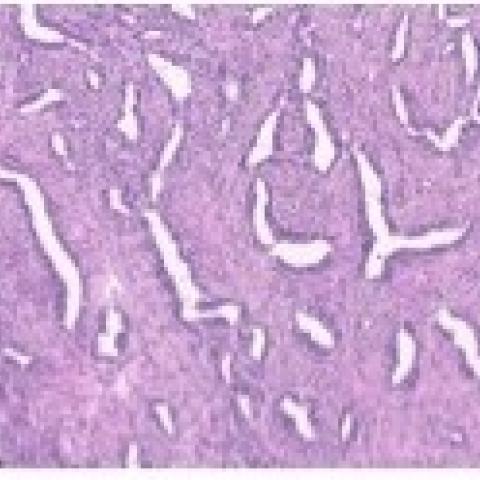
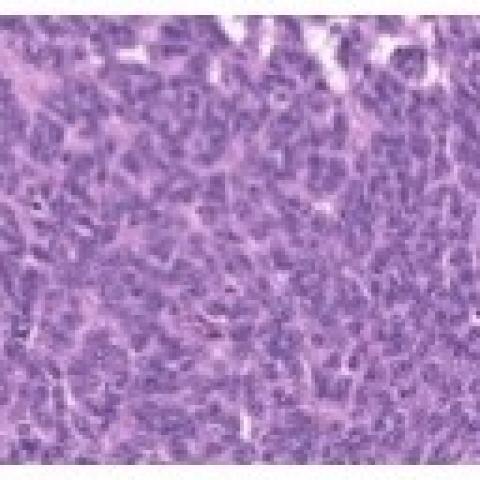
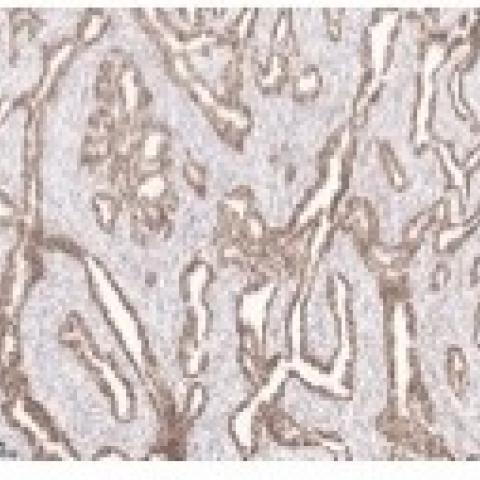
In our case report, the patient underwent a radical orchidectomy shortly after ultrasound findings. Histology confirmed the diagnosis of malignant mesothelioma arising on a background of well differentiated papillary mesothelioma of the tunica vaginalis. [Fig 4a – 4f] [10] The prognosis is largely unpredictable however some studies report a median survival time of 23 months with an overall recurrence rate of 50% and a reported 11% recurrence rate post-radical orchidectomy. [10] Younger patients are reported to have greater survival compared to older patients. [10]
Take Home Message/Teaching Points:
In the assessment of a clinically indolent enlarging painless scrotal mass, imaging features demonstrating a heterogenous vascular mass in association with hydrocele should raise the possibility for malignant transformation of a paratesticular tumour (e.g. WDPM). Chronicity of signs/symptoms does not exclude malignant transformation.
Written informed patient consent for publication has been obtained.
[1] Parcesepe P, Sina S, Zanella C, Pancione M, Giuliani J, Detogni P et al. Case report of a well-differentiated papillary mesothelioma of the tunica vaginalis in an undescended testis with review of the literature. Int J Surg Pathol 2016; 24 (5): 443-447. doi: 10.1177/1066896916628279. Epub 2016 Feb 12. (PMID: 26873338)
[2] Sun M, Zhao L, Lao W, Yu L, Wang J, Well-differentiated papillary mesothelioma: a 17-year single institution experience with a series of 75 cases. Ann Diag Pathol. 2019; 38: 43-50. doi: 10.1016/j.anndiagpath.2018.10.012. Epub 2018 Oct 28. (PMID: 30419426)
[3] Kim MJ, Moon EJ, Park YJ, Roh JW, Park YS, Park SY et al. A case of well differentiated papillary mesothelioma developing malignant mesothelioma with seeding mass on the trocar insertion site of diagnostic laparoscopy and malignant change. Cancer Res Treat 2001; 33(4): 357 - 361. doi: 10.4143/crt.2001.33.4.357. (PMID: 26680808)
[4] Washimi K, Yokose T, Amitani Y, Nakamura M, Osanai S, Noda H et al. Well differentiated papillary mesothelioma, possibly giving rise to diffuse malignant mesothelioma: a case report. Pathol Int 2013; 63(4):220-5. doi: 10.1111/pin.12053. (PMID: 23692423)
[5] Torii I, Hashimoto M, Terada T, Kondo N, Fushimi H, Shimazu K et al. Well differentiated papillary mesothelioma with invasion to the chest wall. Lung Cancer: 2010 Feb;67(2):244-7. doi: 10.1016/j.lungcan.2009.10.004. Epub 2009 Oct 31. (PMID: 1988021)
[6] Costanzo L, Scarlata S, Perrone G, Rossi L, Papa A, Di Matteo FM et al. Malignant transformation of well-differentiated papillary mesothelioma 13 years after the diagnosis: a case report. Clin Respir J 2014; 8(1):124-9. doi: 10.1111/crj.12057. Epub 2013 Nov 26. (PMID: 24118858)
[7] Hannappel TD, DeVried MJ, Hansen NJ. Imaging appearance of cystic and solid mesothelioma of the tunica vaginalis. Radiol Case Rep 2020; 15 (7): 809-811. doi: 10.1016/j.radcr.2020.04.004. eCollection 2020 Jul. (PMID: 32346459)
[8] Mezei G, Chang ET, Mowat FS, Moolgavkar SH. Epidemiology of mesothelioma of the pericardium and tunica vaginalis testis. Ann Epidemiol. 2017;27(5):348–359. e311. (PMID: 28527639)
[9] Kristen Wolanske, Matilde Nino-Murcia. Malignant Mesothelioma of the Tunica Vaginalis Testis - Atypical Sonographic Appearance. J Ultrasound Med 2001, 20: 69-72. (PMID: 11149532)
[10] Plas E, Riedl CR, Pflüger H. Malignant mesothelioma of the tunica vaginalis testis: review of the literature and assessment of prognostic parameters. Cancer. 1998;83(12): 2437–2446. (PMID: 9874447)
| URL: | https://www.eurorad.org/case/16938 |
| DOI: | 10.35100/eurorad/case.16938 |
| ISSN: | 1563-4086 |
This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License.