Teaching Case
SectionHead & neck imaging
Case TypeClinical Cases
Authors
João Diogo Oliveira, Isa Martins
Patient45 years, female
45-year-old Guinean women, with a left supraclavicular tumefaction, associated with cervicalgia, cervical stiffness and limited cervical mobilisation on all planes for 3 years, following a car accident with whiplash injury. Physical examination showed a soft, unpainful, non-pulsatile left supraclavicular lump. Laboratory examinations were unremarkable.
Chest radiography showed left superior mediastinum enlargement with right tracheal deviation.
Ultrasound assessment showed that the supraclavicular tumefaction corresponded to a flowless non-pulsatile cystic image with 5 cm of largest dimensions, surrounded by smaller cystic images.
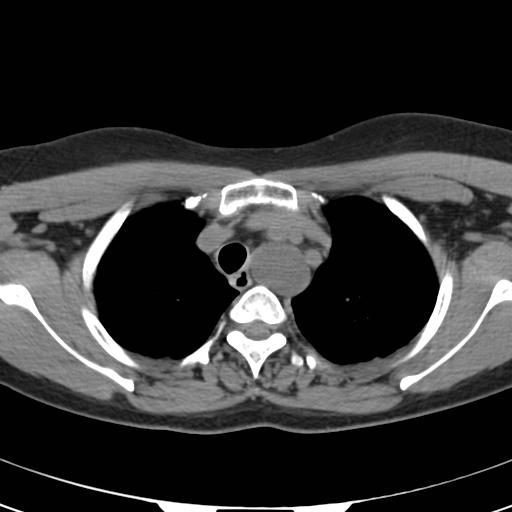
Computed Tomography (CT) revealed in the left supraclavicular topography a bulky cystic image, surrounded by other smaller cystic formations, all interconnected. Concomitant and in contiguity there was a lobulated tubuliform image with identical cystic characteristics in the left posterior mediastinum, with a craniocaudal extension of about 19 cm, and progressive craniocaudal calibre reduction.
T2-weighted magnetic resonance imaging (T2W-MRI) confirmed the massive cystic expansion of the structure located in the posterior mediastinum, located anterior to the spine, to the right of the aorta, to the left to the superior vena cava and posterior to the lobar bifurcation of the trachea, which deviated to the right, communicating with a similar cystic image on the left supraclavicular region.
The thoracic duct is the main collecting vessel of the lymphatic system, draining about three quarters of the lymph into the venous circulation, namely most, although not all, of the subdiaphragmatic regions of the body. It is subject to considerable morphological variation throughout its course, but normally forms from the abdominal confluence of lymph trunks, or in the true cisterna chyli when present, about the first or second lumbar vertebrae, ascends on the right of the aorta and terminates by descending anterior to the first part of the subclavian artery and draining into the junction of the left subclavian vein and the internal jugular vein [1].
Lymphocoele of the thoracic duct is an uncommon abnormality, usually asymptomatic, identified on imaging as cysts on the mediastinum. Less commonly it consists of cystic dilatation of the terminal part of the thoracic duct presenting as a left supraclavicular fossa mass, as in the case presented, constituting the differential diagnosis together with other cystic lesions of the lower cervical region, differentiated by means of appropriate cross-sectional imaging and ultimately by ultrasound-guided FNA [2, 3, 5].
Numerous theories have been suggested to explain the aetiology, and it is accepted to be the result of weakness in the thoracic duct wall following congenital anomalies or an acquired degenerative process caused by inflammation or trauma [1, 2].
On imaging studies the dilated thoracic duct appears as a non-enhancing, tubular/multicystic, multi-compartmental, water density structure (having attenuation slightly lower than the arteries and veins), starting caudally from the upper abdomen, extending cranially towards the mediastinum till its insertion, presenting with areas of more focal dilatation mounting to cyst formation.
Ultrasound-guided FNA may be used to access the lymphatic origin of the supraclavicular mass, demonstrating the aspirate as chyle/lymph, which has a very distinct appearance on gross inspection, exhibiting a milky appearance and a unique composition, having lymphocytes as the predominant cell type and a high concentration of triglycerides and chylomicrons, which makes biochemical analysis confirmatory [1, 4].
No clinical problems derive from it, and thus the clinical significance of the correct recognition of the aetiology of such a neck mass lies in its misidentification as a pathological lesion, which can ultimately lead to inappropriate management, such as unnecessary intervention or secondary complications when surgical intervention is planned, whereas in normal circumstances, conservative management is generally advocated [1, 2].
Written informed patient consent for publication has been obtained.
[1] C E Offiah, BSc, FRCS, FRCR and S Twigg, BSc (2011) Lymphocoele of the thoracic duct: a cause of left supraclavicular fossa. The British Journal of Radiology 84 (2011), e27–e30 (PMID: 21257831)
[2] Mattila PS, Tarkkanen J, Mattila S (1999) Thoracic duct cyst: a case report and review of 29 cases. Ann Otol Rhinol Laryngol 108(5):505–508 (PMID: 10335715)
[3] Lecanu JB, Gallas D, Biacabe B, BonWls P (2001) Lymphocele of the thoracic duct presenting as a left supraclavicular mass: a case report and review of the literature. Auris Nasus Larynx 28:275–277 (PMID: 11489376)
[4] Van Sonnenberg E, Wittich GR (1986) Lymphoceles: imaging characteristics and percutaneous management. Radiology 161:593–596 (PMID: 3538133)
[5] Moesgaard L, Baerentzen S, Mirz F (2007) Cervical thoracic duct cyst: a differential diagnosis of left supraclavicular swelling. Eur Arch Otorhinolaryngol 264:797–799 (PMID: 17297607)
| URL: | https://www.eurorad.org/case/16428 |
| DOI: | 10.35100/eurorad/case.16428 |
| ISSN: | 1563-4086 |
This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License.