Urgent (same day) unenhanced and post contrast multidetector CT

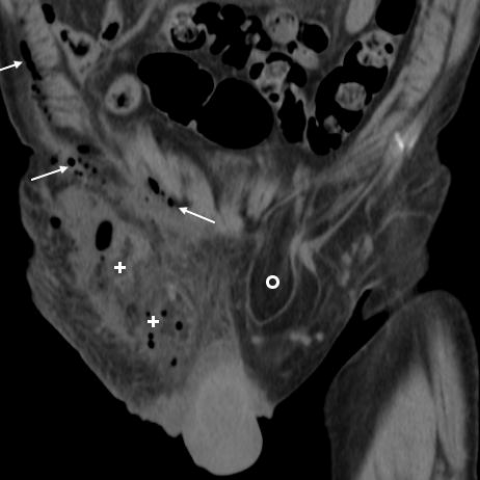





Abdominal imaging
Case TypeClinical Cases
AuthorsTonolini Massimo, MD.
Patient62 years, male
[1] Karthikesalingam A, Markar SR, Holt PJ, et al. (2010) Meta-analysis of randomized controlled trials comparing laparoscopic with open mesh repair of recurrent inguinal hernia. Br J Surg 97:4-11 (PMID: 20013926)
[2] Kingsnorth A (2009) Hernia surgery: from guidelines to clinical practice. Ann R Coll Surg Engl 91:273-279 (PMID: 19416585)
[3] McCormack K, Scott NW, Go PM, et al. (2003) aparoscopic techniques versus open techniques for inguinal hernia repair. Cochrane Database Syst Rev: CD001785 (PMID: 12535413)
[4] Holzheimer RG (2005) Inguinal Hernia: classification, diagnosis and treatment--classic, traumatic and Sportsman\'s hernia. Eur J Med Res 10:121-134. (PMID: 15851379)
[5] Crespi G, Giannetta, Mariani F, et al. (2004) Imaging of early postoperative complications after polypropylene mesh repair of inguinal hernia. Radiol Med 108:107-115 (PMID: 15269694)
[6] Shpitz B, Kuriansky J, Werener M, et al. (2004) Early postoperative evaluation of groins after laparoscopic total extraperitoneal repair of inguinal hernias. J Laparoendosc Adv Surg Tech A 14:353-357 (PMID: 23210400)
[7] Yeung VH, Pearl JM, Coakley FV, et al. (2008) Computed tomographic appearance of prolene hernia system and polypropylene mesh plug inguina hernia repair. J Comput Assist Tomogr 32:529-532 (PMID: 18664837)
[8] arra JA, Revuelta S, Gallego T, et al. (2004) Prosthetic mesh used for inguinal and ventral hernia repair: normal appearance and complications in ultrasound and CT. Br J Radiol 77:261-265. (PMID: 15020373)
[9] Chernyak V, Rozenblit A, Patlas M, et al. (2007) Pelvic pseudolesions after inguinl hernioplasty using prosthetic mesh: CT findings. J Comput Assist Tomogr 31:724-727. (PMID: 17895783)
| URL: | https://www.eurorad.org/case/13123 |
| DOI: | 10.1594/EURORAD/CASE.13123 |
| ISSN: | 1563-4086 |
This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License.