Clinical History
26-year-old lactating female patient (G1, P1) presented with left-sided abdominal pain for the past 3 months. She denied altered bowel habit. Previous medical history recorded childbirth 11 months before, and T shape intrauterine device (IUD) placement 4 months before contrast-enhanced-abdominal CT was performed.
Imaging Findings
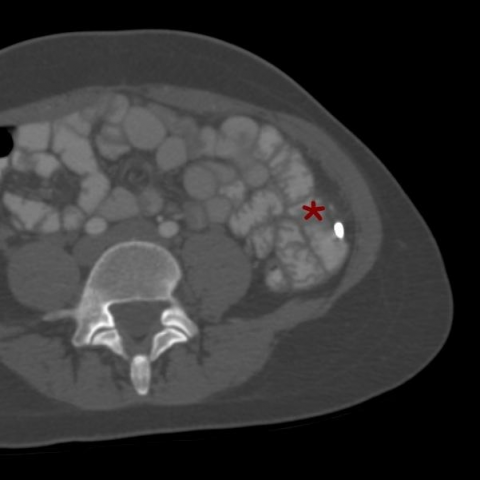
CT revealed metallic IUD-like foreign object located closely next to the small bowel loops in the left lower abdominal quadrant (Fig. 1). 3D virtual reconstruction clarifies IUD recognition (Fig. 2).
Discussion
Since its creation by Richter in 1909, IUDs have been widely accepted as a long-acting reversible contraceptive method [1]. Although considered safe, its usage is not risk-free; relevant complications account for malposition, uterine perforation pelvic inflammatory disease (PID) and unplanned pregnancy [2].
Patients suffering from displaced IUD might experience abdominal pain, fever, mild to severe abdominal tenderness, vaginal discharge and non-specific urinary symptoms [3]. IUD migration can result in perforated hollow viscus, abscess formation or bowel obstruction [4, 5]. Incidence of uterine perforation and migration of IUD into the abdominal cavity through the uterine wall is 1:300 to 1:2500 [4]. Still unclear, risk factors for perforations are thought to be lactancy, birth within the past 6 months, lack of experience of the physician, low oestrogen blood levels or uterine malformations [5]. Other risk factors include previous miscarriages [2].
Diagnosis can be the result of periodical clinical ultrasound (US) check on IUD placement or incidental findings on CT for other indications [5, 6]. Imaging modalities often recommended in the search for missing IUDs are abdominal plain radiographs, which are useful to detect radiopaque objects, abdominopelvic/gynaecological US or abdominal CT (for detailed positioning) [1-6].
IUD should normally be found centrally placed within the uterine cavity [6]. Once displaced or migrated, IUDs effectiveness is reduced, and it is the radiologist's duty to timely and properly inform the referring physician in order to prevent further damage to the patient’s health and avoid undesired if not pathological (ectopic) pregnancy [5].
Required treatment will be based on symptoms or damage suffered. Laparotomy or laparoscopy are effective in retrieving abdominopelvic missing IUDs. If IUDs string is at reach, less invasive approaches (hysteroscopy) can be attempted in an outpatient clinical setting [1-6].
Differential Diagnosis List
Migrated IUD (complete uterine perforation).
Displaced IUD
Embedded IUD
Final Diagnosis
Migrated IUD (complete uterine perforation).