Serial chest radiographs

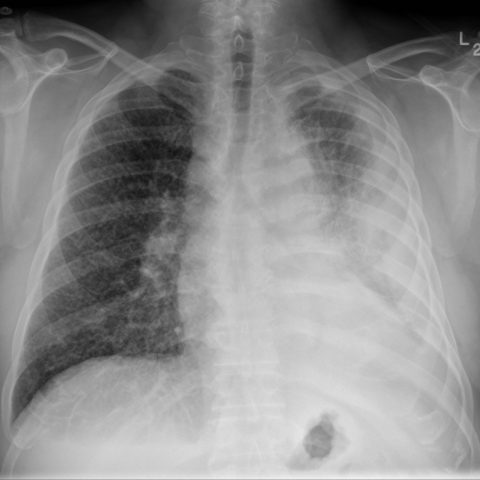
Chest imaging
Case TypeClinical Cases
Authors Patient60 years, male
[1] Wang ZJ, Reddy GP, Gotway MB, Higgins CB, Jablons DM, Ramaswamy M, Hawkins RA, Webb WR (2004) Malignant pleural mesothelioma: evaluation with CT, MR imaging, and PET. Radiographics 24(1):105-19 (PMID: 14730040)
[2] Purek L, Laroumagne S, Dutau H, Maldonado F, Astoul P (2011) Miliary mesothelioma - a new clinical and radiological presentation in mesothelioma patients with prolonged survival after trimodality therapy. Journal of thoracic oncology 6(10):1753-6 (PMID: 21918389)
[3] Livasy CA, Tishko DJ, Maygarden SJ (2003) Miliary pulmonary metastases from a clinically occult pleural mesothelioma. Annals of diagnostic pathology 7(4):249-53 (PMID: 12913849)
[4] Fares M, Abbas O, Jamaleddine G, Bou-Khalil P (2008) Metastases in malignant pleural mesothelioma: a new radiological appearance. Respirology 13(5):746-7. Epub 2008 May 29 (PMID: 18513248)
[5] Huncharek M (1994) Miliary mesothelioma. Chest 106(2):605-6 (PMID: 7774346)
[6] Musk AW (1995) More cases of miliary mesothelioma. Chest 108(2):587 (PMID: 7634910)
[7] Ohishi N, Oka T, Fukuhara T, Yotsumoto H, Yazaki Y (1996) Extensive pulmonary metastases in malignant pleural mesothelioma. A rare clinical and radiographic presentation. Chest 110(1):296-8 (PMID: 8681649)
[8] Uri AJ, Schulman ES, Steiner RM, Scott RD, Rose LJ. (1988) Diffuse contralateral pulmonary metastases in malignant mesothelioma. An unusual radiographic presentation. Chest 93(2):433-4 (PMID: 3338319)
| URL: | https://www.eurorad.org/case/10569 |
| DOI: | 10.1594/EURORAD/CASE.10569 |
| ISSN: | 1563-4086 |