Teaching Case
SectionAbdominal imaging
Case TypeClinical Cases
Authors Patient37 years, male
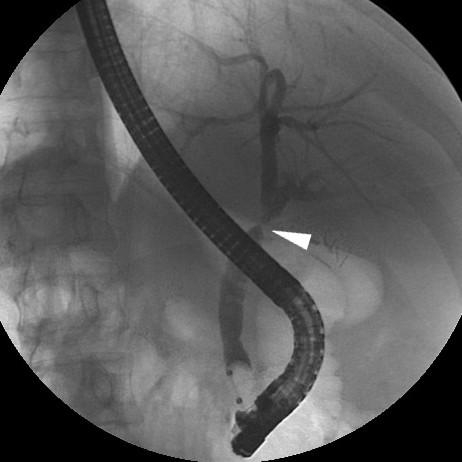
He suffered abdominal pain, vomiting, and hypotension 24 hours after endoscopic positioning of covered metallic biliary stent (Fig. 2).
One month after hospital discharge, the patient was rushed to emergency department with worsening right-sided thoraco-abdominal pain and fever over a week. Urgent MDCT (Fig.4a-g) showed pleural effusion, lung atelectasis, and a huge, predominantly fluid-attenuating (15 Hounsfield Units) subphrenic collection with inflammatory enhancement of the surrounding, compressed liver parenchyma, thin rim-like enhancement, consistent with an abscess. Percutaneous drainage (Fig. 4h..j) yielded 3 liters of stinking pus.
Clinical, laboratory, and imaging (Fig. 5a..c) resolution was obtained. During endoscopic replacement, the biliary stent was not found anymore (Fig. 5d), displaced and probably lost with stools. Contrast (Fig. 5e) and MR cholangiography (Fig. 5f) confirmed persistent iatrogenic biliary stricture with reduced upstream dilatation. Further endoscopic treatment was deemed contraindicated, but the patient refuses proposed surgical revision.
Endoscopic positioning of plastic or self-expandable metal stents is an appealing, minimally invasive treatment for biliary strictures. Alternatively, stenting may be performed through a percutaneous transhepatic or combined approach. Technical and clinical success rates reach 99% and 80% respectively. Clinical effectiveness is generally lower (55-82%) with percutaneous positioning. However, biliary stenting is associated with a significant (39.5%) risk of complications. By far, the commonest complication (25-35% of patients) is stent obstruction, with reported patency rates of 38% and 25% at 2 and 3 years respectively, without significant differences between underlying causes [1-4].
Less common complications include stent misplacement or dislodgement (4-6% of patients), infection (variably presenting as cholangitis, liver abscess and/or sepsis), haemobilia, perforation, stent fracture or collapse [4-6].
As this case with serial occurrences exemplifies, imaging (particularly with multidetector CT in an emergency setting) is necessary to recognize stent-related complications. Complemented with multiplanar reformations, CT provides high-resolution visualization of the stent, whether of plastic or metallic reticular “mesh” material, of the biliary segment where it is located, and of its anatomical relationships. Interpretation of post-procedural studies should review stent type, integrity, patency, and position including proximal and distal extremities. Furthermore, the presence of abnormal findings such as blood, gas, or fluid collections should be noted, as well as signs of inflammatory enhancement or active bleeding [5, 6].
Occurring after a variable time interval, displacement of a biliary stent may be proximal, particularly in patients with malignant obstruction, or alternatively distal to the intestine, that is not unusually asymptomatic. Suggested by clinical and laboratory findings, superinfection may cause septic cholangitis (with thickened enhancing ductal walls), or formation of liver abscess, appearing as a fluid-like collection with peripheral enhancement. Finally, the rare subcapsular or intraparenchymal liver haematoma is recognized by its characteristic unenhanced hyperattenuation [5, 6].
In conclusion, awareness of the wide spectrum of possible complications following bile stent positioning is necessary to correctly interpret early and delayed post-procedural imaging studies, to detect correctable complications, thus sparing patients additional morbidity and mortality [6].
[1] van Boeckel PG, Vleggaar FP, Siersema PD (2009) Plastic or metal stents for benign extrahepatic biliary strictures: a systematic review. BMC Gastroenterol 9:96 (PMID: 20017920)
[2] Matlock J, Freeman ML (2005) Endoscopic therapy of benign biliary strictures. Reviews in gastroenterological disorders 5:206-214 (PMID: 16369216)
[3] Judah JR, Draganov PV (2007) Endoscopic therapy of benign biliary strictures. World J Gastroenterol 13:3531-3539 (PMID: 17659703)
[4] Siriwardana HP, Siriwardena AK (2005) Systematic appraisal of the role of metallic endobiliary stents in the treatment of benign bile duct stricture. Ann Surg 242:10-19 (PMID: 15973096)
[5] Pannu HK, Fishman EK (2001) Complications of endoscopic retrograde cholangiopancreatography: spectrum of abnormalities demonstrated with CT. Radiographics 21:1441-1453 (PMID: 11706215)
[6] Catalano O, De Bellis M, Sandomenico F, et al. (2012) Complications of Biliary and Gastrointestinal Stents: MDCT of the Cancer Patient. AJR Am J Roentgenol 199:W187-196 (PMID: 22826420)
| URL: | https://www.eurorad.org/case/10384 |
| DOI: | 10.1594/EURORAD/CASE.10384 |
| ISSN: | 1563-4086 |