The term popliteal artery entrapment (PAE) syndrome was used for the first time by Love and Whelan [1] in 1965 when they reported two cases of unusual calf pain during exercise and intermittent claudication due to popliteal artery occlusion, as result of an anomaly of the relationship between the popliteal artery and the gastrocnemius muscle. In normal condition, the popliteal artery runs in the middle of the popliteal fossa located between the medial and lateral heads of the gastrocnemius muscle, superficially to the popliteus muscle (Fig 5). Abnormal lateral attachment of the medial head of the gastrocnemius muscle, accessory muscle slips, and any other associated anatomic variants localized above the level of tibial tuberosity can cause external popliteal compression.
Pathophysiologically, flow in the popliteal artery is unimpeded in condition of muscle relax; while during gastrocnemius muscle contraction increased arterial angulation develops leading to flore obstruction. Repeated microtraumas on the arterial wall from compression may produce occlusion of the vessel at the site of entrapment. Midpopliteal arterial occlusion due to thrombosis is an important diagnostic sign and, frequently, collateral genicular arteries develop.
PAE should be considered in any active individual who develops calf claudication during strenuous exercise; it generally affects young men, but can observed also in young, athletic women. Bilaterality of entrapment is described with increasing frequency, and associated venous entrapment can cause development of superficial varicosities.
Angiography can show the typical findings of PAE: medial dislocation of the proximal tract of the popliteal artery, segmental stenosis or occlusion in its midportion, and, sometimes, postenotic dilatation. The main disadvantage of angiography is its inability to analyse extravascular structures [2].
Magnetic resonance imaging (MRI) allows evaluation of both soft tissues and vascular structures: changes in the insertion point of the gastrocnemius muscle, presence of accessory muscular slip, deeper than normal localization of the popliteal vessel, and excessive popliteal fat tissue can be recognized, as well as their relationship with popliteal vessels [2];
Magnetic resonance angiography (MRA) permits quick and noninvasive study of both morphology and patency of the vessel. In some cases, only MR studies performed with stress tecnique (Gradient-echo sequences obtained in axial planes with the leg at rest and during active plantar flexion) are able to show signal loss in the popliteal artery due to actual compression on its wall [3].
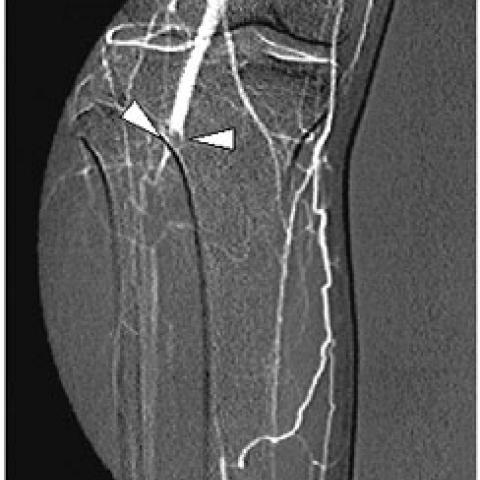
In our case, intra-arterial digital subtraction angiography (DSA) of the right leg performed with homolateral transfemoral approach, revealed a segmental occlusion of the midportion popliteal artery, and normal arterial patency at lower level by genicular collateral development (Fig. 1a)
MRI of the right poplitael fossa, performed by using a circumferential coil (knee coil) in comparative study with the controlateral knee, showed on T1-weighted axial images, an aberrant accessory slip of the medial head of the gastrocnemius muscle, located between popliteal artery and vein, wrapping around the artery and entrapping it (Fig. 3a, 4a), typical features for subtype III of PAE [4], as osservable in Fig. 6. The slip of the medial gastrocnemius muscle had an attachmen more cranial than the lateral gastrocnemius muscle (Fig. 3a) and was not evident in the controlateral knee (Fig. 3c). MRA, performed on axial plane using 2D- FLASH (Fast-Low Angle single-SHot imaging) sequence without contrast medium admnistration and inferior saturation band to study also the popliteal vein, showed medial and anterior displacement of the popliteal artery, confirming the level and extension of arterial occlusion, the nature of external compression, and patency of the popliteal vein (Fig. 4c, 4d).
The patient underwent surgical transection of the accessory muscular slip near its insertion to release the vessel, and to arterial reconstruction using an autogenous greater saphenous vein bypass.
In conclusion, we described a case of monolateral PAE syndrome, studied with DSA, MRI and MRA.